Understanding Disc Inflammation: A Comprehensive Analysis


Overview of Research Topic
Brief Background and Context
Disc inflammation, clinically referred to as discitis, is a condition that often slips under the radar in discussions surrounding spinal health. It is crucial to understand that the intervertebral discs, while primarily known for their role in absorbing shock and facilitating mobility, can also be sites of infection and inflammation. This pathological condition leads to various symptoms, often misattributed to other spinal disorders.
Discitis can affect anyone, but specific populations such as the elderly or those with compromised immune systems may be at higher risk. While acute conditions may arise suddenly, chronic cases might develop insidiously over time. The increasing prevalence of this condition necessitates a thorough understanding, as it can have serious implications for mobility and quality of life in affected individuals.
Importance in Current Scientific Landscape
The significance of disc inflammation within the framework of modern medicine cannot be overstated. Current research has started to peel back the layers on how systemic health issues intersect with spinal disorders. Recent studies have shed light on the role chronic inflammation plays not just in disc degeneration but also in wider systemic diseases. Scientists and medical professionals are increasingly focused on how insights from discitis can inform treatment paradigms for other inflammatory conditions.
Moreover, an interdisciplinary approach is emerging, connecting the fields of immunology, microbiology, and orthopedics, highlighting the need for collaboration in comprehending disc inflammation. By dissecting the complexities of discitis, professionals can develop improved diagnostic methods and therapeutic strategies that enhance patient outcomes.
"The interplay between spinal health and systemic conditions underscores the need for a nuanced understanding of disc inflammation."
Methodology
Research Design and Approach
The analysis of disc inflammation entails a multi-faceted research design, integrating both quantitative and qualitative approaches. Surveys of patient-reported outcomes, along with clinical data reviews, provide a comprehensive view of the symptoms and treatments experienced by individuals affected by discitis. Case studies also play a vital role, allowing for detailed assessments of patient journeys through diagnosis and management.
Data Collection Techniques
Data collection for understanding disc inflammation involves various techniques:
- Clinical Investigations: Conducting MRI and CT scans helps in identifying inflammation within the spinal discs.
- Patient Surveys: Administering detailed surveys on symptoms, treatment efficacy, and quality of life to gather subjective data.
- Biomarker Analysis: Analyzing blood samples for inflammatory markers that provide insight into underlying conditions.
- Literature Review: Examining existing studies allows researchers to build upon established findings and identify gaps in knowledge.
By combining these techniques, a holistic picture of disc inflammation is painted, guiding future research and clinical practice aimed at tackling this often-overlooked condition.
Preamble to Disc Inflammation
Disc inflammation, often referred to as discitis, is a condition that directly impacts the health of the spine yet remains somewhat obscure in common discussions about spinal issues. Understanding this topic is essential, as it brings to light several factors that can significantly alter a person's quality of life.
In this article, we delve into the various layers of disc inflammation, examining its definition, mechanisms, causes, symptoms, and treatments. This insightful analysis is not only beneficial for healthcare professionals but also invaluable for students, educators, and researchers who aim to grasp the nuances of this condition.
Definition and Overview
Disc inflammation primarily refers to the swelling or irritation of the intervertebral discs. These discs serve as the cushions between the vertebrae in the spine, absorbing shocks and enabling flexibility. When these discs become inflamed, they may cause significant pain and discomfort, affecting mobility and overall well-being. Though discitis can occur at any age, its prevalence seems to increase with advancing age, particularly among those who engage in high-impact activities or have certain underlying health conditions.
Importance of Understanding Disc Inflammation
A comprehensive understanding of disc inflammation is crucial for multiple reasons:
- Early Detection: Recognizing the early signs and symptoms can lead to timely intervention, potentially avoiding serious complications.
- Informed Treatment Decisions: Knowledge of the mechanisms behind disc inflammation enables healthcare providers to determine the best treatment approach tailored to the individual’s needs.
- Preventive Measures: Understanding the risk factors associated with discitis empowers individuals to make lifestyle choices that promote spinal health.
"Proactive understanding and intervention can significantly enhance recovery outcomes in patients with disc inflammation."
By exploring disc inflammation in detail, we aim to shed light on its multifaceted nature, aiding not just in academic comprehension but also in practical application for those affected or involved in the sphere of spinal health.
Anatomy of the Spine
Understanding the anatomy of the spine is crucial in the context of disc inflammation, commonly known as discitis. The spine is a complex structure that plays a pivotal role in supporting the body, protecting the spinal cord, and facilitating movement. By grasping how the spine is constructed and functions, we can discern how disc inflammation disrupts these processes. Moreover, an in-depth knowledge of spinal anatomy lays the groundwork for recognizing how various conditions, including discitis, emerge and evolve.
Structure of Intervertebral Discs
Intervertebral discs are unique structures located between each pair of vertebrates in the spine, acting like shock absorbers. They consist of two primary components: the nucleus pulposus and the annulus fibrosus. The nucleus pulposus, which is the inner gel-like core, allows the disc to withstand pressure from various angles, while the annulus fibrosus, a tougher outer layer, aids in maintaining the disc's shape and integrity.
The overall health of these discs is essential for ensuring proper spinal alignment and mobility. When discussing disc inflammation, it’s vital to acknowledge how degeneration or trauma can lead to inflammation and subsequently impact the individual’s overall spinal function.
Function of Discs in Spinal Health
Discs serve several key functions that are integral to spinal health:
- Shock Absorption: The gel-like nature of the nucleus allows it to absorb and distribute stress as the body moves, protecting the vertebrae from wear and tear.
- Facilitating Movement: Intervertebral discs enable a range of motions in the spine, from twisting to bending. This flexibility is essential for everyday activities, from mundane tasks to athletic pursuits.
- Support and Stability: Discs help to keep the vertebrae aligned, contributing to overall spinal stability. When inflammation occurs, this balance may be disrupted, leading to pain and physical limitations.
"A well-functioning spinal disc is fundamental to optimal mobility and quality of life. Disruption in disc structural integrity inevitably leads to significant discomfort and dysfunction."
By comprehending the anatomy and function of intervertebral discs, we begin to appreciate the complexity of discitis and its ramifications. Knowing how these discs operate sheds light on the importance of identifying, diagnosing, and addressing any inflammation that may arise. It is through this understanding that effective management strategies can be formulated, ultimately improving patient outcomes.
Pathophysiology of Disc Inflammation
Understanding the pathophysiology of disc inflammation is crucial for grasping the broader implications of this condition on spinal health. Disc inflammation, known medicaly as discitis, can stem from various triggers and has significant consequences if left untreated. By delving into the mechanisms and biological processes underlying this condition, individuals can appreciate how vital it is to recognize symptoms early and seek appropriate treatment.
Mechanisms of Inflammation
Disc inflammation begins with a cascade of responses in the body that aims to protect and heal. When intervertebral discs sustain injury or become infected, the vasodilation process kicks in, wherein blood vessels widen to increase blood flow to the affected area. This process allows immune cells to migrate to the site, where they can combat any harmful agents.
Several factors contribute to the inflammation cycle:
- Physical strains: If a person lifts something heavy or maintains poor posture, it can put undue stress on the spinal discs.
- Infections: Pathogens, like bacteria or fungi, can invade the discs. They create by-products that trigger inflammation.
- Degenerative changes: The natural aging process results in wear and tear. Over time, discs lose hydration, making them less resilient and more prone to inflammation.
As inflammation progresses, it may lead to further structural damage to the disc, spurring a vicious cycle that complicates recovery.
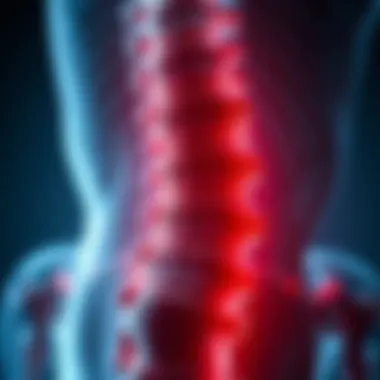
"Understanding the mechanisms of inflammation is key to developing effective treatment options."
Inflammatory Cytokines Involved
Cytokines are small proteins that play a pivotal role in cell signaling during immune responses. In cases of disc inflammation, certain cytokines become overly active, exacerbating inflammation. Two significant cytokines often noted are Interleukin-1 (IL-1) and Tumor Necrosis Factor Alpha (TNF-alpha). Their presence indicates a heightened inflammatory state, and they can even modulate pain pathways in the spinal region.
The implications of these cytokines include:
- IL-1: This cytokine promotes inflammation and can attract immune cells to the injury site, often amplifying the pain experience.
- TNF-alpha: It works both to initiate inflammation and to modify the healing processes. High levels of TNF-alpha are often correlated with increased pain and reduced functional recovery.
Understanding these cytokines doesn't just inform us about the inflammatory response but also hints at potential treatment avenues. Targeting specific cytokines through biologic therapies may provide a new way to manage symptoms effectively and reduce inflammation.
Research into the specific roles cytokines play in disc inflammation is ongoing, presenting exciting possibilities for developing new treatment protocols that are more targeted and effective.
For further reading, you might find these resources helpful:
With a clearer picture of the pathophysiology of disc inflammation, medical professionals and patients alike can make informed decisions about treatment and management strategies.
Common Causes of Disc Inflammation
Understanding the causes of disc inflammation is crucial for identifying treatment strategies and preventative measures. Discitis, as it’s often referred to, can manifest through various means that may range from bacterial infections to injuries. By exploring each factor in depth, we not only uncover the roots of the issue but also initiate proactive measures to ensure spinal health.
Infectious Agents
Infectious agents are a prominent cause of disc inflammation, and they significantly shift the focus from simple mechanical issues to complex pathological involvement. Bacteria like Staphylococcus aureus and Mycobacterium tuberculosis are known culprits. These organisms can either invade the disc directly or spread through the bloodstream from other parts of the body. An individual with a compromised immune system might be at a higher risk.
Symptoms may present as fever, localized pain, and swelling, oftentimes misattributed to other musculoskeletal complications. If you suspect an infection, rapid intervention is key, as untreated cases can lead to severe complications, including abscess formation or permanent damage to the spine. Understanding the link between infections and disc inflammation can significantly impact treatment outcomes.
Non-Infectious Causes
Non-infectious causes of disc inflammation bring in a whole different set of problems. These can include autoimmune disorders, degenerative diseases, and metabolic conditions. In autoimmune disorders, the body’s immune system mistakenly targets the discs, leading to inflammation. Conditions like rheumatoid arthritis can trigger discitis-like symptoms without involving pathogens.
Furthermore, degenerative diseases such as disc degeneration or loss of disc height can predispose the spine to inflammation. Poor nutrition, particularly deficiencies in Vitamin C or D, may also contribute to the weakening of the disc structure, spurring inflammation.
- Key considerations in this context include:
- Awareness of personal health history.
- Regular monitoring for symptoms.
- Comprehensive approaches that target underlying conditions.
Traumatic Factors
Traumatic factors can lead to disc inflammation in both acute and chronic scenarios. A sudden injury, such as a fall or impact during sports activities, may directly damage the disc material, triggering an inflammatory response. Chronic trauma, often seen in manual laborers or athletes, may also lead to micro-tears within the disc, compounding inflammation over time.
The body’s response to trauma often results in pain and reduced mobility. Recognizing the signs of trauma-related inflammation is essential for swift treatment and rehabilitation.
Factors like:
- Repetitive stress
- Poor posture
- Lack of proper equipment in sports
can exacerbate the condition further.
Addressing these causes involves a multi-faceted approach, involving appropriate physical therapy, ergonomic adjustments, and possible medicinal support.
Understanding these common causes of disc inflammation not only sheds light on the complexity of the illness but also empowers individuals to take informed steps towards better spine health. By knowing what can inflame the discs, practitioners and patients alike can strategically manage and hopefully prevent the incidence of discitis.
Symptoms and Clinical Presentation
Understanding the symptoms and clinical presentation of disc inflammation is essential not just for diagnosis but also for effective management of the condition. Discerning the specific symptoms can significantly influence treatment pathways, influencing overall outcomes for the patient. Moreover, the way symptoms manifest can vary widely among individuals due to factors like age, health, and the underlying cause of inflammation. A clear grasp of these elements makes a world of difference when navigating the complexities of disc inflammation.
Typical Symptoms of Disc Inflammation
When discussing typical symptoms, it’s vital to recognize that disc inflammation commonly presents itself in a variety of ways. Some of the most frequently reported symptoms include:
- Localized Back Pain: This is often the first and most noticeable symptom. Patients may describe this as a persistent ache or sharp pain, usually centered in the lower back.
- Radiating Pain: The discomfort can extend beyond the back and may radiate into the legs or arms, depending on the affected area of the spine. This radiating pain can sometimes be described as tingling or numbness.
- Stiffness: Many individuals report an increase in stiffness, especially after periods of inactivity. This stiffness can make movements difficult, leading to a decreased range of motion.
- Weakness in Limbs: In some cases, weakness in the arms or legs may surface, often correlating with the nerves being affected by the inflamed disc.
- Inflammatory Symptoms: Additionally, systemic symptoms like fever or chills might occur if the inflammation is due to an infectious agent.
Understanding these symptoms is paramount for individuals who suspect they may be dealing with this condition. Often, what begins as a minor discomfort can escalate into a more severe problem if left unchecked. Regular monitoring and appropriate responses to these symptoms can serve as a proactive approach to spinal health.
Differentiating Symptoms from Other Conditions
One of the challenges in clinical practice is distinguishing the symptoms of disc inflammation from other spinal or neurological conditions. Several overlapping symptoms can lead to confusion.
For instance, nerve compression from other issues, such as herniated discs or degenerative spine diseases, will often present similarly. The key differences might lie in:
- Symptom Onset: Symptoms from disc inflammation frequently arise more acutely, often following an identifiable trigger such as physical exertion or injury.
- Location of Pain: While disc inflammation pain is typically localized, pain from conditions such as sciatica may follow distinct nerve paths due to different underlying causes.
- Accompanying Symptoms: Other conditions may not exhibit the same systemic inflammatory symptoms (fever, chills) associated with disc inflammation.
"In the realm of spinal health, a misdiagnosis could lead to ineffective treatments and prolonged suffering. Understanding symptomatology warrants careful consideration."
For clinicians, a thorough patient history and physical examination, combined with appropriate diagnostic imaging, can clarify the nuances between these conditions. This meticulous process not only aids in providing a correct diagnosis but also ensures the most efficient and effective treatment plan is put in place worthy of discourse.
Diagnostic Approaches
The realm of diagnosing disc inflammation is both intricate and vital. Understanding the various diagnostic methods allows healthcare professionals to accurately identify this condition, which often presents subtle and non-specific symptoms. Early diagnosis can significantly alter the trajectory of treatment and recovery, so unpacking these approaches gives a clearer picture of their importance in managing disc inflammation.


Clinical Evaluation
A thorough clinical evaluation serves as the cornerstone for diagnosing disc inflammation. It usually begins with a detailed patient history, focusing on the onset and course of symptoms. Healthcare providers will often inquire about factors such as:
- Pain characteristics: Location, intensity, and duration
- Functional limitations: Daily activities that are affected
- Prior medical history: Previous spinal issues or surgeries
- Potential risk factors: Any recent infections or traumas
This initial evaluation helps in forming a hypothesis about the possible underlying causes of the symptoms, guiding further testing. Following history-taking, a physical examination is typically conducted. The provider will assess muscle strength, reflexes, and any neurological deficits, often looking for signs of irritation or nerve involvement that might indicate inflammation.
Imaging Techniques
Following the clinical evaluation, imaging techniques are essential in confirming the diagnosis. Commonly utilized methods include:
- X-rays: While they might not show soft tissue clearly, X-rays can help identify bone spurs, fractures, or other bony abnormalities that could contribute to disc inflammation.
- MRI (Magnetic Resonance Imaging): This is typically the gold standard for visualizing the soft tissues, including the intervertebral discs. An MRI can illustrate the presence of inflammation, herniated discs, or other pathologies impacting the spinal structure.
- CT Scans (Computed Tomography): In cases where MRI is unavailable or contraindicated, a CT scan provides another detailed view, particularly of bony structures that may be affecting disc health.
These imaging techniques not only assist in diagnosis but also aid in planning treatment strategies by highlighting the extent and nature of the condition.
Laboratory Tests and Biomarkers
While imaging techniques give structural insights, laboratory tests and biomarkers serve to shed light on the biological activity within the body. Blood tests can be instrumental in detecting markers of inflammation, such as:
- C-reactive protein (CRP): Elevated levels may indicate an inflammatory process occurring.
- Erythrocyte sedimentation rate (ESR): This test helps identify the presence of inflammation, though it is less specific.
- Blood cultures: In cases where infectious discitis is suspected, identifying any pathogens in the blood can be crucial.
Overall, the combination of clinical evaluations, imaging, and laboratory tests provides a comprehensive view, enhancing the diagnostic accuracy for disc inflammation. The integration of these approaches ensures that healthcare providers can formulate effective, personalized treatment plans, reducing the chances of complications and promoting better recovery outcomes.
“The stakes are high; accurate diagnosis influences the path for effective treatment and patient recovery.”
Treatment Options for Disc Inflammation
Disc inflammation can be a thorn in the side of many individuals, affecting not just physical health but overall quality of life. Hence, the exploration of treatment options is imperative in managing this condition effectively. Approaches to treatment vary widely, accounting for the severity of inflammation, underlying causes, as well as the patient’s individual health profile. Understanding these options can equip those affected by disc inflammation with the knowledge needed to make informed decisions and ultimately guide them toward better health outcomes.
Conservative Management Strategies
Often the first line of defense in tackling disc inflammation lies in conservative management strategies. These methods are generally non-invasive and can provide substantial relief for many.
Rest and Activity Modification
Giving the spine a break is fundamental in this phase. Too much movement can exacerbate the inflammation. Avoiding high-impact activities and taking breaks during tasks can aid recovery. On the flip side, some gentle exercises might be encouraged when symptoms improve, keeping the body in shape without straining the back.
Physical Therapy
Working with a skilled physical therapist can be a game changer. Personalized rehabilitation programs targeting core strengthening and flexibility can be designed to stabilize the spine. Techniques such as heat and cold therapy, ultrasound, and electrical stimulation might also find a place in this routine. Patients have found that simple stretches can ease discomfort and improve mobility over time.
Lifestyle Adjustments
Making some changes in daily habits can also yield benefits. Maintaining a healthy weight can reduce unnecessary pressure on the spine. Ergonomic workspaces can promote better posture, and practicing mindfulness can help manage pain perception. All these changes may contribute positively to recovery from disc inflammation.
Medications and Therapies
For many facing a tougher battle with disc inflammation, medications and therapies become critical allies.
Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
Over-the-counter options like ibuprofen or naproxen can help tame inflammation and manage pain effectively. While they offer symptomatic relief, it's essential to not over-rely on them, as prolonged use might lead to side effects such as gastrointestinal issues.
Corticosteroid Injections
In more persistent cases, corticosteroid injections directly into the affected area can provide significant relief. This therapy helps reduce swelling and pain, often leading to a respite from bothersome symptoms. However, it is crucial for patients to discuss the risks and benefits with their healthcare provider each step of the way.
Alternative Therapies
In addition to conventional medicines, some individuals explore complementary therapies like acupuncture and chiropractic care. Though evidence is mixed, many report subjective improvements in symptoms. Thus, these options may worth a try for those desiring a holistic approach.
Surgical Interventions
In situations where conservative management fails or the inflammation brings about severe complications, surgical interventions might become necessary.
Discectomy
This procedure involves removing a portion of the damaged disc to relieve pressure on surrounding nerves. By alleviating the source of inflammation, many experience significant pain reduction thereafter.
Spinal Fusion
In instances where multiple discs are affected, spinal fusion could be the solution. This surgery connects two or more vertebrae, ultimately reducing motion and stabilizing the spine. Though it sounds alarming, many have found renewed strength and reduced discomfort post-surgery.
Artificial Disc Replacement
A newer approach involves replacing a damaged disc with an artificial one. This method aims to maintain motion in that area while relieving pain. While this option is not suitable for everyone, results have been promising for select patients.
In summary, treating disc inflammation is not a one-size-fits-all approach. Individuals must work closely with healthcare professionals to tailor a treatment plan that aligns with their specific circumstances. Each option mentioned has its own set of benefits and risks, which need to be carefully weighed in the quest for relief. As research advances, new techniques and therapies continue emerging, bringing hope for more effective management of this condition in the future.
Prognosis and Long-Term Outcomes
Understanding the prognosis and long-term outcomes of disc inflammation is crucial for patients and healthcare professionals alike. This aspect not only provides insights into recovery expectations but also shapes treatment approaches and patient management. Knowing what factors can influence recovery helps guide individual treatment plans and improve outcomes, making proactive measures and realistic goal-setting possible.
Factors Influencing Recovery
Recovery from disc inflammation can be a multifaceted journey, impacted by myriad factors, both intrinsic and extrinsic. Recognizing these elements is essential for tailoring treatment and managing expectations. Here are some key considerations:
- Patient’s Overall Health: A person's general health condition plays a considerable role. Those with underlying health problems, like diabetes or obesity, might experience slower recovery times. Maintaining a healthy lifestyle can make a world of difference.
- Severity of Inflammation: The level of inflammation present at the time of diagnosis can influence recovery duration. Severe cases may need more aggressive treatment strategies compared to milder forms.
- Comorbidities: Other medical conditions can complicate recovery. For instance, individuals with chronic pain conditions may find it harder to manage symptoms related to disc inflammation.
- Adherence to Treatment Plans: Following prescribed therapies and lifestyle changes is paramount. Those who commit to physical therapy or medication as advised often experience a quicker and more effective recovery.
- Age Factor: Simply put, younger patients generally have a better prognosis. Age can affect healing capabilities, as older individuals may have decreased regenerative potential.
In summary, taking into account these factors can lead to tailored, effective treatment plans that may help in speeding up recovery times.
Potential Complications
Despite the potential for a positive outcome, there can also be complications arising from disc inflammation. These complications may impact long-term health and quality of life. Some notable risks include:
- Chronic Pain: A significant portion of patients may continue to experience persistent pain even after treatment. Managing this pain is crucial as it can heavily influence daily life and overall well-being.
- Nerve Damage: In severe cases where the inflammation affects nearby nerves, patients can develop nerve damage. Symptoms can include numbness or weakness in the limbs, complicating recovery further.
- Recurrence: Individuals who have suffered from disc inflammation may be at risk for recurrent episodes, especially if preventive measures aren't taken.
- Emotional Distress: Living with chronic pain or other complications can lead to anxiety or depression. The psychological aspects should not be overlooked; they require equal attention in treatment protocols.
- Impact on Lifestyle: Limitations caused by ongoing symptoms may affect physical activity levels or even professional life, leading to broader implications on a person’s quality of life.
Long-term management and awareness of the potential complications are vital for navigating the patient journey post-diagnosis.
Preventive Measures
Preventive measures play a crucial role in maintaining spinal health and preventing disc inflammation. By understanding and implementing specific strategies, individuals can significantly reduce their risk of developing debilitating conditions that affect the spine. Preventive measures encompass a range of lifestyle choices and awareness practices that promote a healthier spine and overall well-being. This section aims to highlight the necessity of these preventive strategies, their benefits, and critical considerations when it comes to spinal health.
Lifestyle Modifications for Spine Health
Embracing lifestyle modifications is pivotal for spinal health, particularly in the context of preventing disc inflammation. Here are some key adjustments individuals can consider:
- Ergonomic Workplace Setup: Whether you're typing away at a desk or lifting heavy objects, ensuring that your workspace is ergonomically sound can relieve undue stress on the spine. Chairs with proper lumbar support and adjustable desks can make a world of difference.
- Balanced Nutrition: A diet rich in anti-inflammatory foods can strengthen spine health. Incorporating leafy greens, fatty fish, nuts, and fruits can help mitigate inflammation and support overall well-being.
- Weight Management: Excess weight places additional pressure on the spinal discs, making them more susceptible to inflammation. By maintaining a healthy weight through balanced nutrition and exercise, individuals can alleviate some of this burden.
Making these lifestyle changes may seem taxing at first, but they can lead to substantial benefits in the long run. Here, small adjustments can yield big results.
Importance of Physical Activity
Physical activity is another cornerstone of spine health that cannot be understated. Regular movement not only strengthens the muscles surrounding the spine but also enhances flexibility and reduces stiffness.
- Strength Training: Building core strength is vital for spinal support. Engaging in exercises that target the core muscles can help stabilize the spine and prevent injuries.
- Low-Impact Aerobics: Activities such as swimming or cycling can improve cardiovascular health while being gentle on the joints and spine. These forms of exercise promote blood flow, enhancing recovery and reducing inflammation.
- Stretching and Flexibility: Simple stretching routines can vastly improve mobility and help keep the spine supple. Regular stretching can help prevent the tightness that contributes to disc inflammation.
"An ounce of prevention is worth a pound of cure."
By integrating regular physical activity into daily routines, individuals not only safeguard themselves against disc inflammation but also contribute to their overall health and wellness. The body thrives on movement, and a commitment to physical activity lays the groundwork for a healthier spine.
The Role of Research in Understanding Disc Inflammation
Research serves as the backbone of medical advancement, shedding light on complex conditions such as disc inflammation. It allows us to decipher the intricate mechanisms at play, identify effective treatments, and ultimately improve patient outcomes. By delving into the multifaceted nature of disc inflammation, researchers contribute not just to the academic realm but also to practical healthcare solutions that can change lives.
First and foremost, understanding the role of research is pivotal for several reasons:
- Identification of Mechanisms: Research elucidates the biological and pathological processes involved in disc inflammation. This understanding might lead to targeted therapies that address the root causes rather than just alleviating symptoms.
- Development of Treatment Protocols: As studies examine various treatment modalities, they help establish evidence-based protocols. These protocols guide clinicians in choosing the most effective methods tailored to individual patients.
- Raising Awareness: Academic pursuits in this field foster discussions within the medical community and promote the dissemination of knowledge to the public, which is essential for recognizing early signs of disc inflammation.
To truly grasp the complexities of disc inflammation, it becomes crucial to highlight pivotal studies and findings in the area.
Recent Advances in Medical Research
Recent advancements in medical research have significantly transformed our perspective on disc inflammation. Studies have shifted from broader understanding to focusing on specific areas such as microbial involvement and genetic predisposition. Here are some noteworthy developments:
- Microbiome and Inflammation: Recent studies indicate that microbial communities in the spine may contribute to inflammatory processes. The interplay between bacteria and the immune system in the spinal region is an area that’s drawing attention for its potential therapeutic implications.
- Regenerative Medicine: Research into regenerative therapies, like stem cell injections, shows promise in promoting healing in inflamed discs. These approaches aim to restore disc function and provide long-term relief by harnessing the body’s own healing abilities.
- Genetic Factors: Investigating genetic markers has opened new frontiers in understanding susceptibility to disc inflammation. Knowing how genetic factors may predispose individuals to spinal diseases could lead to tailored preventive measures.
These advances not only enrich our understanding but also enhance clinical practices, giving hope for effective intervention.
Future Directions in Discitis Studies
Looking ahead, several promising avenues of research emerge that could redefine our approach to managing disc inflammation:
- Targeted Anti-Inflammatory Therapies: Developing specific drugs targeting the cytokines involved in disc inflammation may provide more effective relief with fewer side effects.
- Longitudinal Studies: More extensive longitudinal studies to track the natural progression of discitis could unveil patterns that lead to predictive tools for early diagnosis and management.
- Interdisciplinary Research: Collaboration among orthopedists, rheumatologists, and microbiologists can facilitate a more holistic understanding of the condition. Such interdisciplinary approaches can give rise to innovative treatment regimes that combine various specialties.
Through diligent research, the medical community can foster deeper insights into disc inflammation, leading us closer to effective prevention and intervention strategies.
In short, research is not merely a tool, but a vital component of our ongoing quest for better treatments for disc inflammation. As we forge ahead, every discovery holds the potential to enhance patient care and ultimately improve the quality of life for those affected by this condition.
For more detailed information on the advancements in disc inflammation, you can explore resources like National Institutes of Health, PubMed, and World Health Organization.
Understanding the role of research in disc inflammation remains a priority for medical professionals, driving the quest for knowledge and innovation.
Ending
The exploration of disc inflammation in this article underscores its critical nature in the realm of spinal health. As a condition that can lead to various complications if left unchecked, recognizing the symptoms and understanding the underlying mechanisms becomes vital for patients and healthcare providers alike. This conclusion serves to encapsulate the salient points discussed throughout the article while also emphasizing the importance of continued attention to this complex subject.
Summarizing Key Points
Throughout our analysis, several key points emerged that are essential in understanding disc inflammation:
- Definition and Impact: Disc inflammation, often referred to as discitis, is characterized by the inflammation of intervertebral discs, leading to pain and potential dysfunction in the spine.
- Causes and Triggers: Understanding both infectious and non-infectious causes, along with traumatic factors, helps delineate the multifaceted nature of the condition.
- Symptoms and Diagnosis: A variety of symptoms, including localized pain and neurological signs, can indicate disc inflammation. Differentiating these symptoms from other spinal disorders is crucial for accurate diagnosis.
- Management and Treatment: Options range from conservative approaches—such as physical therapy and pain management—to surgical interventions in severe cases, depending on the severity and underlying cause.
- Preventive Strategies: Emphasizing lifestyle changes can play a significant role in enhancing spinal health and preventing disc inflammation.
The Importance of Continued Research
Continued research in the field of disc inflammation is paramount for several reasons:
- Advancements in Understanding: As scientists delve deeper into the pathophysiology of discitis, more targeted therapies could emerge, ultimately leading to improved outcomes for patients.
- Identification of New Treatment Modalities: Innovative research can reveal novel therapeutic strategies that may mitigate the need for invasive procedures.
- Public Awareness and Education: Increasing awareness about disc inflammation can empower individuals to seek timely interventions, thus reducing the risk of chronic pain and disability.
- Interdisciplinary Approaches in Medicine: Collaborations among various fields—such as immunology, orthopedics, and rehabilitation—can forge new pathways for understanding and managing disc inflammation effectively.
In closing, this comprehensive analysis not only sheds light on the multifaceted anatomy of disc inflammation but also highlights an urgent call for ongoing research. Effective management and prevention of this condition will undoubtedly have significant implications for spinal health and overall well-being.
"Understanding and addressing disc inflammation can transform lives—by recognizing it early, we can tackle its repercussions head-on, ultimately leading to healthier spine and life overall."
For further insights and information, readers may refer to resources like WebMD and Mayo Clinic.



